
Pituitary Tumour Surgery In Hyderabad

Pituitary tumour surgery is a specialised neurosurgical procedure designed to treat abnormal growths affecting the pituitary gland, a small but vital structure located at the base of the brain. The pituitary gland regulates essential hormones that control growth, metabolism, reproduction, and stress response. Tumours in this area, though often benign, can cause significant hormonal imbalances and neurological symptoms due to their location near critical structures including the optic nerves and carotid arteries.
Most pituitary tumours are addressed through minimally invasive endoscopic approaches that allow precise tumour removal while preserving normal pituitary function and surrounding structures. Surgery may be recommended to restore hormonal balance, relieve pressure on adjacent nerves, or address symptoms caused by tumour growth. With advances in endoscopic techniques and intraoperative imaging, pituitary surgery has become safer and more effective.
“Pituitary surgery demands precision and detailed anatomical knowledge. The goal is complete tumour removal while protecting the delicate structures that control vision and vital hormonal functions.”
Dr. Sai Shiva Tadakamalla, Brain & Spine Surgeon
Pituitary tumour surgery is performed by Dr. Sai Shiva Tadakamalla, a consultant neurosurgeon in Hyderabad with specialised training in skull base surgery, using advanced endoscopic and microsurgical techniques focused on hormonal preservation, visual protection, and optimal patient outcomes.

What Is Pituitary Tumour Surgery?
Pituitary tumour surgery involves the surgical removal of abnormal growths from the pituitary gland or surrounding sellar region. The pituitary gland sits in a bony cavity called the sella turcica at the skull base, positioned just below the optic nerves and surrounded by important blood vessels and brain structures.
The primary surgical approach is the transsphenoidal technique, performed through the nasal passage using endoscopic visualisation. This minimally invasive method avoids external incisions and provides direct access to the pituitary region. In select cases involving larger tumours with significant extension, a transcranial approach may be considered. The surgical goal depends on tumour type and may include complete removal, hormonal normalisation, or decompression of affected structures.
Consult a neurosurgeon in Hyderabad for comprehensive evaluation and treatment planning for pituitary tumours.
Types Of Pituitary Tumours Treated
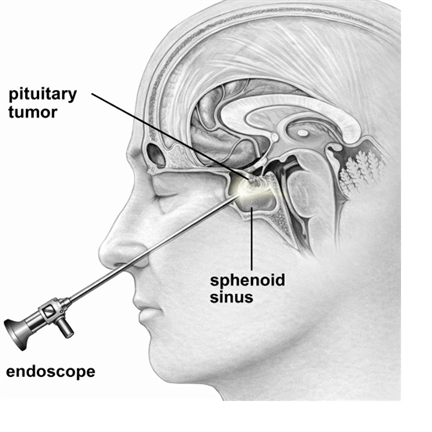
Endoscopic Pituitary Surgery
Advanced minimally invasive technique performed through the nasal passages using high-definition endoscopic equipment. This approach provides excellent visualisation of the pituitary region, allows precise tumour removal while preserving normal gland function, and offers faster recovery with no external incisions.
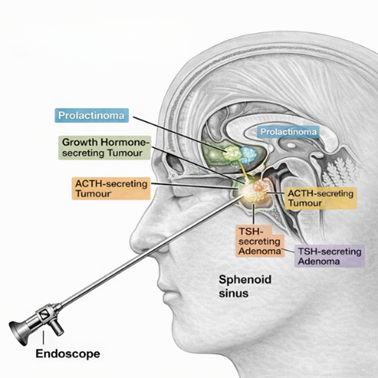
Hormone-Secreting Tumours
Treatment of functioning adenomas that produce excess hormones including prolactinomas, growth hormone-secreting tumours causing acromegaly, ACTH-secreting tumours causing Cushing’s disease, and TSH-secreting adenomas. Surgery aims to normalise hormone levels and eliminate associated symptoms.
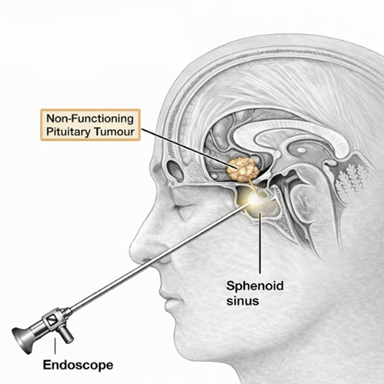
Non-Functioning Pituitary Tumours
Management of adenomas that do not produce excess hormones but cause symptoms through mass effect on surrounding structures. Surgery focuses on relieving pressure on the optic nerves to restore vision, decompressing the normal pituitary gland, and preventing further growth-related complications.
Symptoms Of Pituitary Tumours
Pituitary tumour symptoms vary depending on tumour size, hormone production, and involvement of surrounding structures. Common presentations include:
- Visual field defects or vision loss due to optic nerve compression
- Persistent headaches, often frontal or behind the eyes
- Hormonal imbalances causing irregular menstruation, infertility, or sexual dysfunction
- Excessive growth or acromegaly features in adults
- Weight gain, easy bruising, and muscle weakness in Cushing’s disease
- Fatigue, low blood pressure, and cold intolerance from pituitary insufficiency
- Galactorrhea or inappropriate breast milk production
- Changes in facial features or hand and foot size
- Double vision or eye movement problems
- Unexplained weight changes or mood alterations
The decision for surgery is individualised based on careful assessment of tumour characteristics, patient symptoms, hormonal status, and overall health in consultation with endocrinologists and ophthalmologists when needed.
When Is Pituitary Tumour Surgery Recommended?
Pituitary tumour surgery may be recommended in several clinical situations:
Visual Symptoms
When tumours compress the optic nerves causing visual field defects or progressive vision loss, urgent surgical decompression is often necessary to prevent permanent damage.
Hormonal Excess
For functioning tumours producing excessive hormones that cannot be adequately controlled with medication, surgery offers definitive treatment and potential cure.
Tumour Growth
Progressive enlargement on serial imaging, particularly in non functioning adenomas, may warrant surgical intervention to prevent future complications.
Pituitary Apoplexy
Sudden bleeding within a tumour causing severe headache, vision loss, or altered consciousness requires emergency surgical decompression, similar to other brain surgery emergencies.
Failed Medical Therapy
When medications are ineffective, poorly tolerated, or require lifelong use with significant side effects, surgery may be preferred.
The decision for surgery is individualised based on careful assessment of tumour characteristics, patient symptoms, hormonal status, and overall health in consultation with endocrinologists and ophthalmologists when needed.
Surgical Approaches For Pituitary Tumours
Endoscopic Transsphenoidal Surgery
The preferred minimally invasive approach for most pituitary tumours. Surgery is performed through the nasal passages using advanced endoscopic equipment, allowing excellent visualisation and precise tumour removal without external incisions. This technique offers faster recovery, minimal discomfort, and reduced complications.
Microscopic Transsphenoidal Surgery
An alternative approach using an operating microscope through a small incision beneath the upper lip or within the nostril. This traditional technique remains valuable for certain tumour configurations and provides effective results.
Transcranial Approach
Reserved for large tumours with significant extension into surrounding brain areas or unusual anatomical configurations. This approach allows direct visualisation of the tumour and surrounding structures when transsphenoidal access is insufficient. In such cases, surgical management may overlap with brain tumour surgery.
Recovery After Pituitary Tumour Surgery
Recovery following pituitary surgery is generally well tolerated with appropriate post operative care:
Hospital Stay
Most patients remain hospitalised for 8 to 10 days for monitoring of fluid balance, hormone levels, and nasal healing. Some may require longer observation depending on individual circumstances.
Activity Resumption
Light activities can usually resume within one to two weeks. Strenuous activity, heavy lifting, and nose blowing are avoided for several weeks to allow proper healing.
Follow Up Care
Regular monitoring with MRI imaging and hormonal testing is essential to assess surgical results, detect any tumour recurrence, and optimise long term outcomes.
Hormonal Management
Temporary or permanent hormone replacement may be needed. Endocrine assessment is performed before discharge and during follow up to ensure appropriate hormonal balance.
Visual Recovery
Patients with pre operative visual symptoms often notice improvement within days to weeks as pressure on the optic nerves is relieved, though complete recovery may take longer.
Why Choose Dr. Sai Shiva Tadakamalla For Pituitary Tumour Surgery?
Specialised Skull Base Training
Fellowship training in complex skull base surgery at a premier national institute with focused expertise in pituitary and sellar region pathology.
Advanced Endoscopic Techniques
Proficient in modern minimally invasive endoscopic approaches that reduce recovery time and surgical morbidity.
Multidisciplinary Collaboration
Works closely with endocrinologists, ophthalmologists, and radiation oncologists to provide comprehensive pituitary tumour care.
Evidence Based Decision Making
Treatment recommendations guided by current evidence, international guidelines, and individualised patient needs.

Dr. Sai Shiva Tadakamalla, Brain & Spine Surgeon in Hyderabad
“Successful pituitary surgery requires not just technical skill but also careful coordination with hormone specialists and thoughtful long term planning for each patient’s unique situation.”
Schedule a consultation with an experienced neurosurgeon in Hyderabad to discuss personalised pituitary tumour treatment options.
Frequently Asked Questions
Are all pituitary tumours cancerous?
No, the vast majority of pituitary tumours are benign adenomas. Pituitary carcinomas are extremely rare. However, even benign tumours require treatment when they cause symptoms or hormonal problems.
Will I need hormone replacement after surgery?
This depends on preoperative pituitary function, tumour size, and surgical extent. Some patients require temporary replacement while others may need lifelong therapy. Hormonal status is carefully monitored and managed.
Can vision problems be reversed with surgery?
Many patients experience significant visual improvement after surgical decompression of the optic nerves, particularly when surgery is performed before permanent damage occurs. Earlier intervention generally leads to better visual outcomes.
How long does pituitary surgery take?
Surgery duration varies based on tumour size and complexity, typically ranging from 2 to 4 hours. More extensive tumours may require longer operative time.
What is the success rate of pituitary surgery?
Success rates vary depending on tumour type, size, and invasion. For microadenomas, cure rates often exceed 80-90 percent. Larger tumours may have different outcomes and sometimes require additional treatment.
Will the tumour come back after surgery?
Recurrence risk depends on tumour type and extent of removal. Regular MRI surveillance is important for early detection. Some patients may benefit from additional therapy such as radiation if complete removal was not possible.
